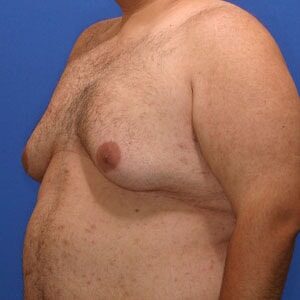
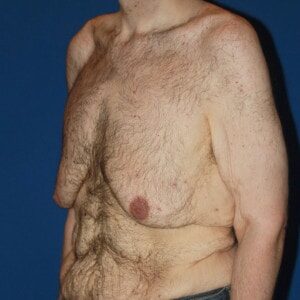
Gynecomastia Types
The purpose of categorizing the different gynecomastia types is to determine which treatment is best based on the underlying problem. Dr. Cruise created the “Cruise Classification System” to demonstrate how each of the 6 gynecomastia types vary. Click below to see a detailed explanation and outline of treatment options for each type of gynecomastia.
A Classification system is only useful if it guides treatment. This is my roadmap for determining the best treatment for each of the 6 types of gynecomastia with the goal of providing the best possible results.
– Dr. Cruise
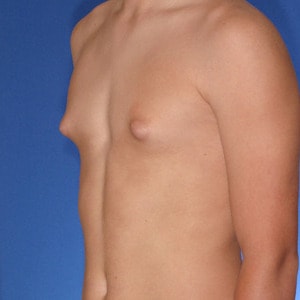
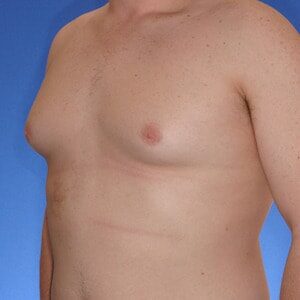
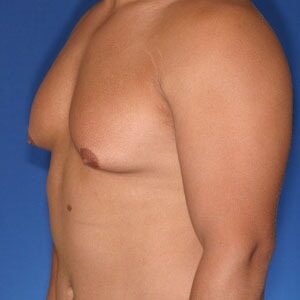
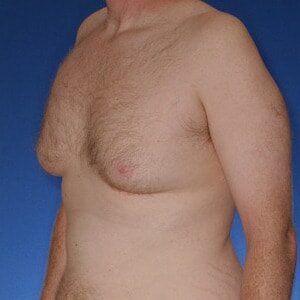
Cruise Classification System – 6 Types of Gynecomastia
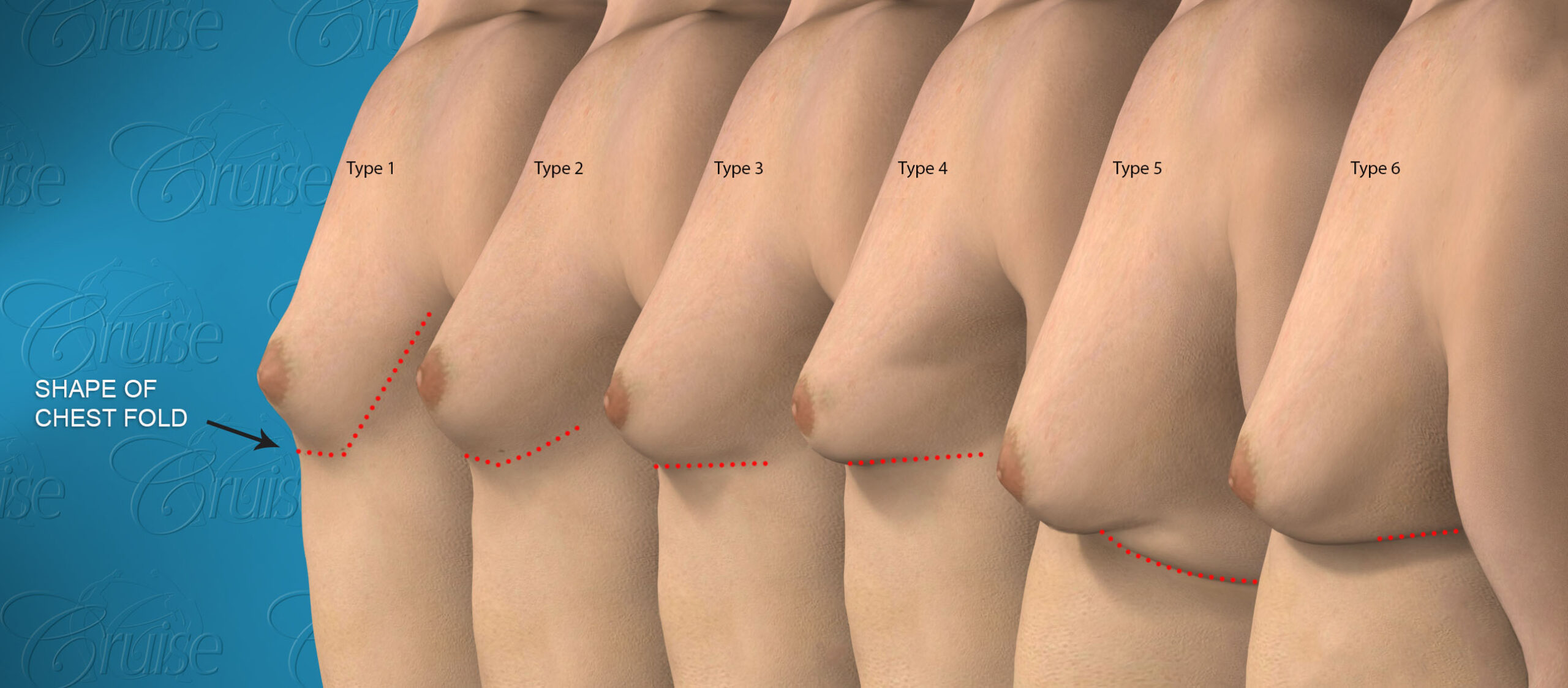
Notice the progressive increase in skin laxity. This excess skin will change the type of surgery necessary to properly correct the problem.
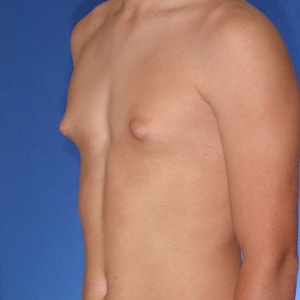
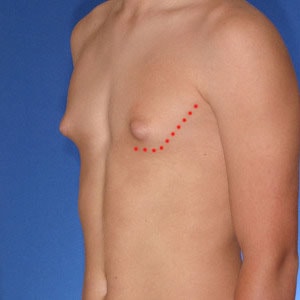
- Type 1
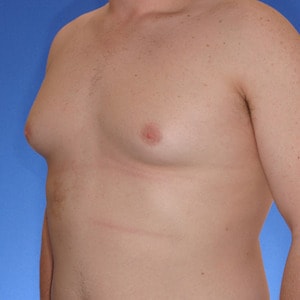
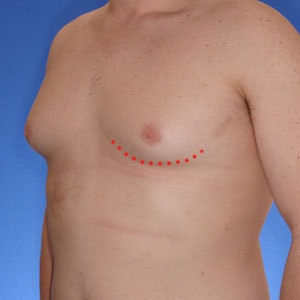
- Type 2
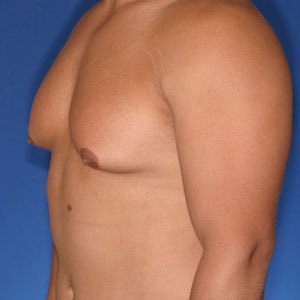
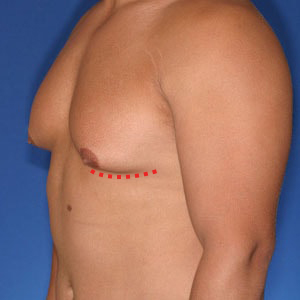
- Type 3
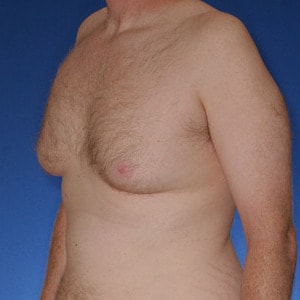
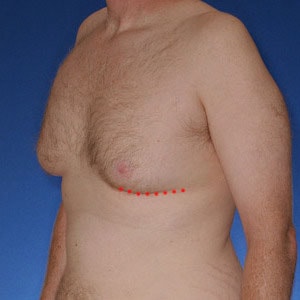
- Type 4
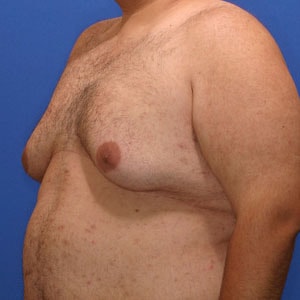
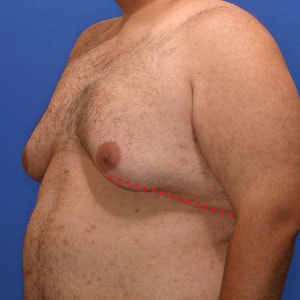
- Type 5
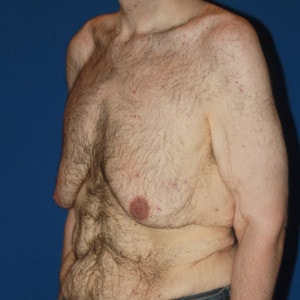
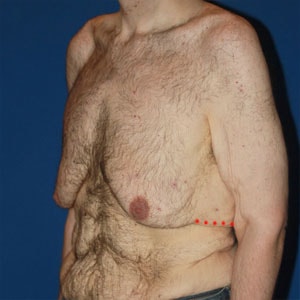
- Type 6
Shorter Incision vs Optimal chest shape
This is without doubt the biggest struggle gynecomastia patients have. However, it really only applies to patients with Gynecomastia Types 3 or 4.
Patients with Gynecomastia Types 1 and 2 do not have much to worry about as their skin is already tight. Their incision will be limited to around the areola. There are some Type 1’s and 2’s that have very low nipples. In these patients, nipple elevation is usually required to prevent the nipple from “falling off the pectoralis border”. If this happens, the nipple is falls into the chest fold and it looks like it is “cratered”. Clearly, not desirable. This requires a superior areola incision which is slightly more visible but still not an issue.
Gynecomastia Types 5 and 6 are discussed in their section. But suffice to say, incisions are unavoidable and are what make these results so spectacular.
Type 3’s and Type 4’s are where incision choices make the biggest difference. This decision process is discussed in those sections. However, experience has shown time and time again that chest shape trumps incisions with rare exceptions. In addition, it is important to consider how you will look not only in 2-3 years but also in 2-3 decades. Any skin laxity now will be a real problem as you age while incisions will be nothing but a faded memory. It is better to have time on your side.
“With time, incisions fade while saggy skin gets worse”
– Dr. Cruise
Having said that, shorter incisions should be considered on patients who have a significant risk of very poor scarring. This includes history of true keloids and skin that hyper-pigments significantly. This needs to be discussed on a case by case basis taking into account patient goals.
Schedule a Consultation
If you are experiencing Gynecomastia Types 1-6, Dr. Cruise has over 20 years of experience and is ready for you to schedule a free consultation. Give us a call at (949) 644-4808 or fill out the online contact form to take the next steps to correct your gynecomastia.