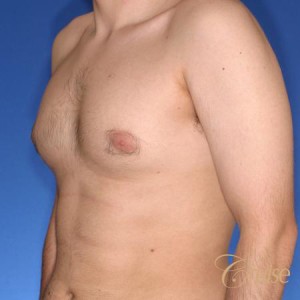
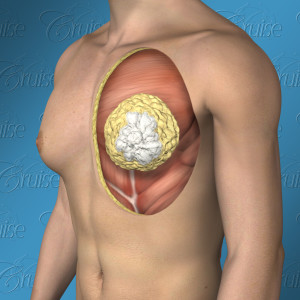
Type 2 Gynecomastia - Rounded Chest
1. Overview
Average cost: $8,500- $9,500
Recovery: 2 Days sedentary work, 4-6 weeks heavy labor
3. Anatomy of Type 2
Firm, white, glandular tissue located almost exclusively underneath the nipple/areola
Type 2 Overview
Rounded Chest
Definition
Breast tissue – extends over pectoralis muscle border
Nipple position – at or above pectoralis border
Chest fold shape – tight skin, rounded chest fold
Most common demographic: 16 – 35 years old, frustrated young adults.
Characterized by excess breast tissue located throughout the lower chest with relatively tight skin. Type 2 has a rounded looking breast shape.
Surgery Information
Anesthesia: Typically performed under local anesthesia in the office, however, general anesthesia is available as well.
Cost: Average cost under local anesthesia is $8,500 – $9,500. The cost will vary if combined w/ other procedures or performed under general anesthesia.
Consultation fee: Charged upon scheduling a consultation.
Recovery: 2 days for sedentary work, 4-6 weeks if the job requires heavy labor.
Cruise Classification System
Based on over 2500 gynecomastia surgeries, Dr. Cruise has classified gynecomastia into 6 different types. Each type is unique in its own way and must be treated differently. The purpose of the Cruise Classification System is to:
- Classify gynecomastia type
- Define patient goals
- Outline optimal treatment plan
“A classification system is only useful if it outlines a treatment plan.” – Dr. Cruise
Cruise Classification System – 6 Types of Gynecomastia
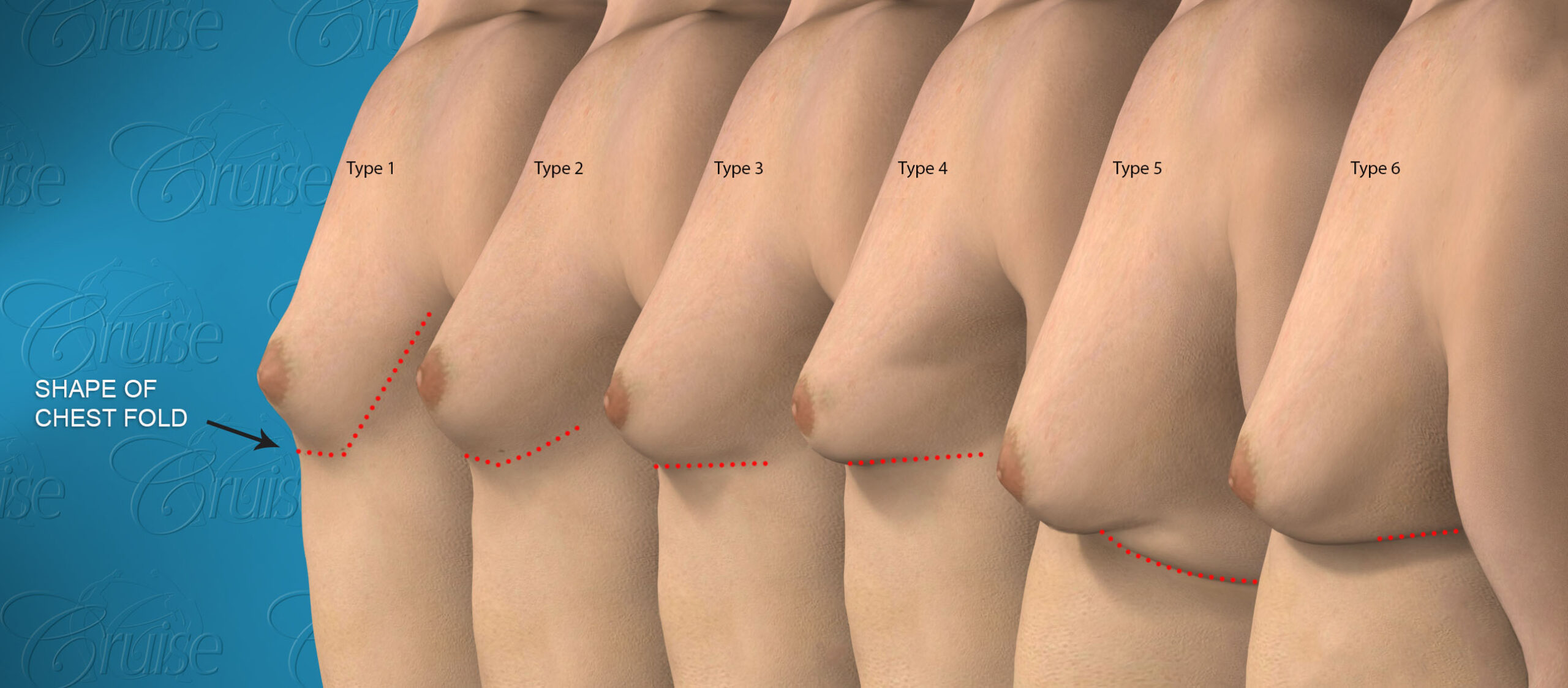
Notice the progressive increase in skin laxity. This excess skin will change the type of surgery necessary to properly correct the problem.
-
Type 1
Breast tissue – under nipple/areola only
Nipple position – above border of pec. muscle
Lateral chest fold – tight, straight
-
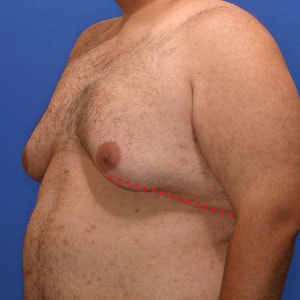
Type 2
Breast tissue – extends over chest fold
Nipple position – above border of pec. muscle
Lateral chest fold – tight, rounded
-
Type 3
Breast tissue – extends over chest fold
Nipple position – 0 to 2 cm. below border of pec. muscle
Lateral chest fold – mild laxity, horizontal
-
Type 4
Breast tissue – extends into axilla
Nipple position – >1.5 cm below border of pec. muscle
Lateral chest fold – small breast roll in front of arm pit
-
Type 5
Breast tissue – extends into axilla
Nipple position – ≥ 2 cm below border of pec. muscle
Lateral chest fold – breast roll extends to the back of arm pit
-
Type 6
Breast tissue – extends into axilla
Nipple position – ≥ 2cm below border of pec. muscle
Lateral chest fold – breast roll extends around to back
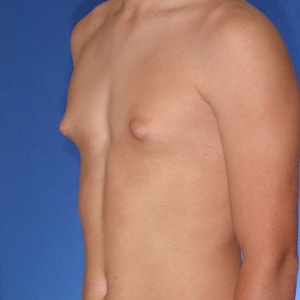
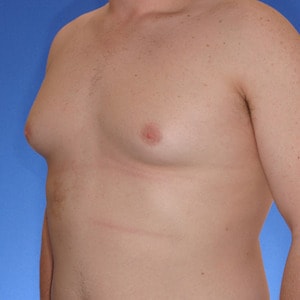
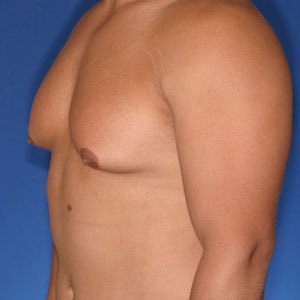
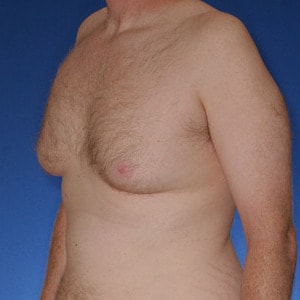
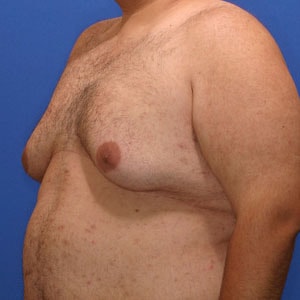
What is Type 2 Gynecomastia?
Type 2 Gynecomastia has breast tissue that extends over the pectoralis muscle causing a feminine, rounded appearance.
Fortunately, Type 2’s have tight skin which acts like a compression garment – holding the breast tissue tight and flat. In fact, this compression may be so effective that it makes the gynecomastia tissue appear as well developed muscle to causual observers. However, the rounded, undefined lower pectoralis border is what gives it away as breast tissue. Another way to distinguish breast tissue from muscle is to squeeze all the tissue directly below the areola with your thumb and index finger. Breast tissue will have a firm, gritty texture. If left untreated, over time the weight of the breast tissue will cause the skin to relax and likely progress to Type 3 or Type 4.
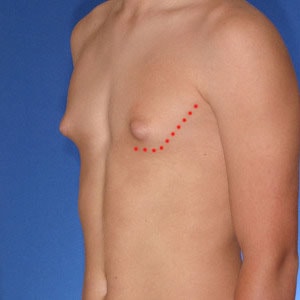
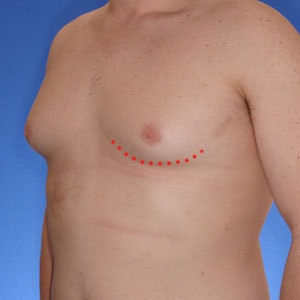
Anatomy of Type 2 Gynecomastia
-
Typical appearance
Type 2 is characterized by a rounded, feminine appearance of the chest fold as well as greater overall breast tissue size. This full, rounded appearance is particularly bothersome because it is particularly noticeable with fitted shirts.
-
What's going on underneath
While Type 2's typically have significantly more volume than type 1's; however, they often have similar puffy nipple. Therefore, having puffy nipple does not mean you are a Type 1. As you can see, the biggest difference is that the breast tissue drapes over the pectoralis muscle border. This disrupts the muscle definition and overall masculine appearance.
Optimal Results for Type 2 Gynecomastia
Unfortunately, the clinical definition for optimal results for gynecomastia is virtually non-existent; even in plastic surgery literature. Type 2 Gynecomastia does not necessary mean easiest. In fact, Type 2 patients are very particular and do not tolerate complications such as persistent puffy nipple, cratering, contour irregularities, etc. Type 2 patients are typically in very good physical shape to begin. While puffy nipple is of the major concern, there are many other aspects of Type 2 gynecomastia that absolutely need to be addressed in order to not only achieve optimal result but, more importantly, avoid complications.
“Achieving optimal results and avoiding complications requires both expertise and a plan”
– Dr. Cruise
- Read more...
The most common cause of poor outcomes is not having this plan. Unfortunately, gynecomastia treatment has never been given the same attention that most other plastic surgery procedures. This over-sight is the reason for this site. To create the fertile infrastructure to allow both patients and surgeons to communicate their experience. To exchange ideas and show not only what works but also what doesn’t.

Anatomy of a Masculine Chest
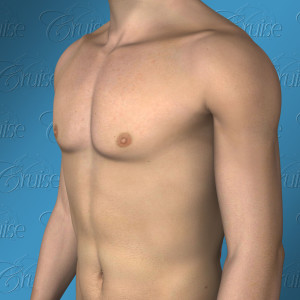
External view of optimal result
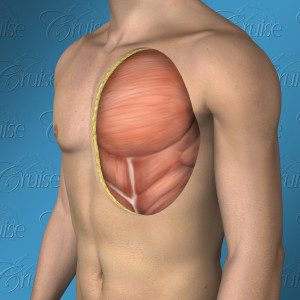
Inside view of optimal result
What defines “Optimal Results?”
The Cruise classification accurately defines “where you are.” Now, we need to clearly define in surgical terms “where you want to go.”
With this is mind, we asked Dr. Cruise to outline the most important aspects that need to be addressed when surgically treating Gynecomastia Type 2 and what they should ideally look like.
Eight Components
-
1. Chest shape - masculine, flat and defined
Overall, a masculine chest is full and powerful above the nipple but ripped and defined below. The key is to create muscle definition, flatten the nipple, yet keep the chest area above the areola normal thickness. Thinning too much will create a “fragile” appearance and worse, may create contour irregularities. The goal is to flatten the chest so that you can confidently wear tight white T-shirts and to create a V shape from both the back and front view.
-
2. Nipple position
Ideally, the nipple should be 1-2 cm above the pec. border (pectoralis major muscle). However, it is perfectly acceptable even if it is located directly on the border as long as it sits on a convex (not concave) surface. This is particularly true with body builders or men with large pec. muscles as it gives the low lying nipple a bigger base to sit on. However, when it sits below the pec. border it begins to face downward or worse it falls into the chest fold which is concave. Sitting in the chest fold often gives the appearance of “cratering.”
-
3. Areola size, projection and shape
The areola is the dark, pigmented skin around the nipple. Areola size is proportionate to chest size. Ideally, it should 25-35 mm and lay flush with the surrounding skin. However, slight elevation is common. Most people do not consciously realize it but areolas are usually wider than they are tall. A perfectly round areola is not ideal and an areola that is taller than it is wide may even appear unusual or “surgical”. This is particularly relevant with types 4,5 and 6 which usually require reducing and re-positioning the nipple with a free nipple graft. A protruding nipple is common with puffy nipple due to the pressure from the swollen breast tissue below. However, there are situations where the nipple is simply enlarged. Fortunately, reducing the nipple by excision is straight forward, low cost, little down time and very effective.
-
4. Pec. border definition
Ideally, the pectoralis major muscle should be defined and straight with the skin wrapping around it into a well defined chest fold and then into a defined arm pit hollow. Excess breast tissue, fat and/or saggy skin will blur this border and create a round, feminine appearance.
-
5. Arm pit
Should have sculpted appearance with a well define hollow at its apex. The borders of the pec. major in front and the latissimus dorsi in back should be well defined giving a V shape to the upper body. Excess fat/saggy skin can fill the arm pit creating an uncomfortable fullness in armpit and a saggy breast roll just below. Creating a sculpted axilla and a V shape appearance to the upper body is one of the most rewarding parts of gynecomastia surgery yet it is usually overlooked as not being part of the gynecomastia. It is important for your surgeon to understand that the goal of surgery is to create a V shaped, masculine chest and not just to remove breast tissue. I can not tell you have powerful the results are when you create a sculpted pec., lat. and arm pit. It is truly life changing.
-
6. Three Fat pockets – pre-axillary, axillary and breast roll
Ideally, there should not be any fat pockets. There are three common fat pockets that need to be evaluated and removed if present.
- Pre-axillary fat – located just in front of the armpit.
- Axillary fat – located within the arm pit itself and
- Breast roll fat – located just below the arm pit and creates a fullness or breast roll. They blur pec., arm pit and lat. definition and disrupts V shape upper body that defines masculinity.
-
7. Breast rolls
-
8. Back rolls
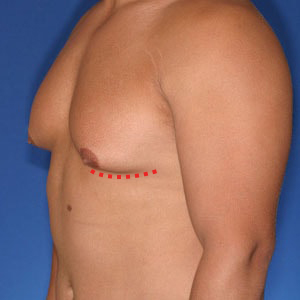
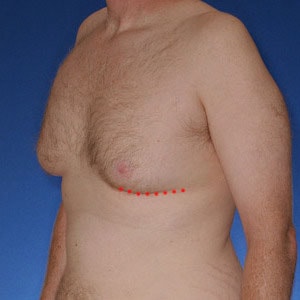
Shorter Incision vs Optimal Chest Shape
Type 2 gynecomastia patients do not have much to worry about extra incisions as their skin is already tight. Their incision will be limited to around the areola. There are some Type 2’s that have very low nipples. In these patients, nipple elevation is usually required to prevent the nipple from “falling off the pectoralis border.” If this happens, the nipple falls into the chest fold and it looks like it is “cratered.” Clearly, not desirable. This requires a superior areola incision which is slightly more visible but still not an issue. As one of the best gynecomastia surgeons in the world, Dr. Cruise is extremely skilled with his incision techniques.
Surgical Treatment Options
Incision visibility is less of an issue with Type 2 Gynecomastia compared to the other types. This is because even the most aggressive incision still remains within the areola. Incision choices for Type 2 are:
Type 2 Incision Options
Crescent excision means that a 1/4″ to 1/2″ crescent shaped piece of skin is removed just below and above the areola. This does several good things beyond tightening the chest skin. More importantly, it pulls the areola tight similar to getting the wrinkles out of a bed sheet. This little maneuver has a large impact in getting rid of excess skin that has been stretched over time. It also flattens the lower and upper chest skin mildly so that it better wraps around the pec. border improving definition. One incision is located above and second below the areola.
Crescent incisions, however, create skin margins that do not line up exactly. The side toward the areola will always be shorter than its counterpart. When sutured together this length mismatch will create mild bunching that takes a little longer to fade away than a linear incision would.
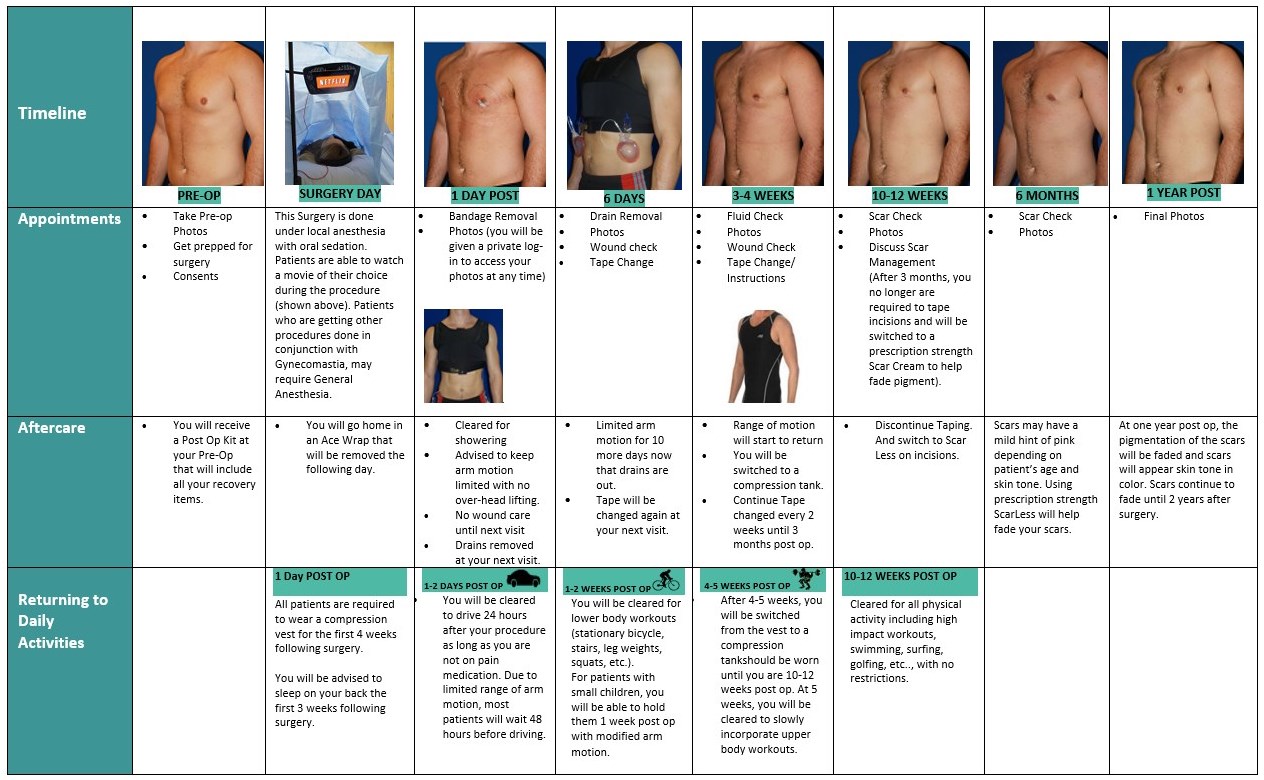
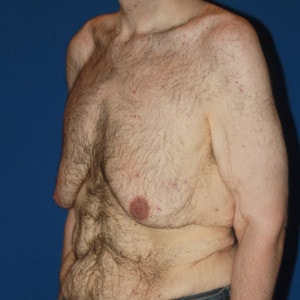
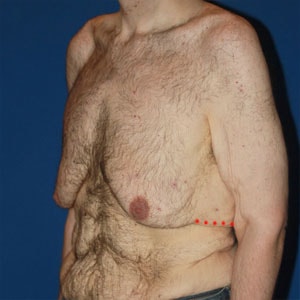
Gynecomastia Before & After Photos
View our gallery of before and after photos to see the results from Type 2 Gynecomastia surgery. Remember, each patient is unique and results will vary from person to person.
Type 2 Before & After Examples
Emotional Cost of Gynecomastia
The pain and suffering associated with gynecomastia is unlike any other condition in plastic surgery and perhaps in all of medicine. The range of its impact is stunning. Some men (usually older) can be relatively unaffected while others (usually the younger) can be completely devastated and even suicidal.
- Read more...
Unfortunately, because of the stigma associated with it, it is not always readily apparent what your loved one may be experiencing. In fact, the men or more commonly pubescent teenagers, who are most deeply effected go to great lengths to suffer alone. The Internet becomes the only one they can talk to. This dangerous combination of deep emotional pain and isolation makes them particularly vulnerable to exploitation. Exploitation that takes the form of the literally thousands of “miracle” cures that have no medical merit to the more nefarious types looking to take advantage of the the emotionally weak.
Patient Perspective – common feelings associated with patients who have Type 2 Gynecomastia:
- Feels trapped and alone.
- Thoughts of being abnormal/different.
- Unaware condition has a name: Gynecomastia. (However, internet is changing this).
- Younger living w/ parents; may or may not discuss with them.
- If still in school, gynecomastia can be anywhere from uncomfortable to unbearable.
- Wide spectrum of outward expression from normal to:
-
- Hunched neck and shoulders.
- Downward gazing head/eyes.
- Uncomfortable with eye contact
- Becoming more and more reclusive for no obvious reason.
- Feels depressed.
- Lacks confidence, poor self-image.
- Negative impact on other aspects of life including school, work, family, friends, relationships.
Parent Perspective – signs of concern
- Observe. Is your son avoiding outdoor/shirtless activities he use to love?
- Has he started wearing a shirt at the pool/beach?
- Is he becoming reclusive/negative?
- Is he declining in academics?
- Does he come up with excuses to avoid PE or hanging out with friends?
- More obvious – is he being ridiculed by schoolmates and even friends, being called titty twister, or being a subject of “man boobs” jokes, etc?
- Is he starting to wear shirts that are loose fitting? Does he wear hoodies or jackets more often?
- Do you see him routinely pulling his shirt away from his chest?
Most of the time, your son will not want to “speak up” about his embarrassment of Gynecomastia. In addition, he probably does not even know there is a name for the condition that he suffers with. The key here is to educated the child on Gynecomastia. The best way is to first approach your child and ask them why he has not been going to the pool or avoiding shirtless situations. If you have a specific example, use it. Have this conversation in a private place where he has your full attention and feels safe to open up. Using media coverage such as the article in Parenting OC is a good way to break the ice. Some intro statements could be:
- I noticed that you did not want to go swimming with your friends last week, I know how much you love to swim, so I just wanted to check in and make sure all is ok.
- It seems like you have been not wanting to participate in activities that require you to be shirtless and I just wanted to let you know that if you are feeling self-conscious about an element of your body, I am here if you want to talk about it.
- A lot of body changes can happen during the teen years and if anything is happening to your body that you are not comfortable with or embarrassed about, please let me know as I may be able to help you. I just read an article in Parenting OC about Gynecomastia and I thought it would be good for you to look it over to see if this is something you may be dealing with.
Very important: Let your child know that you are judgement free.
Spouse/Significant Other Perspective – signs of concern
- Observe. Is your spouse/significant other avoiding outdoor/shirtless activities he use to love?
- Does he wear shirt at the pool/beach?
- Is he more reclusive/negative?
- Does he avoid going to the gym or working out in general?
- Or, is he obsessed with working out/body building and dieting?
- Do you see him researching and/or buying”miracle” cure supplements?
- Is he wearing over-sized clothing? Routinely tugging his shirt away from his chest?
- Does he become embarrassed when you see him without his shirt on?
- Is your sex life declining?
Schedule a Consultation
If gynecomastia surgery is a procedure that you are considering or you just want to learn more about your options, fill out our online contact form and you will be contacted with the next steps to resolve your gynecomastia. Feel free to also call our office at (949) 644-4808.
Video Testimonals - a Partner & a Patient